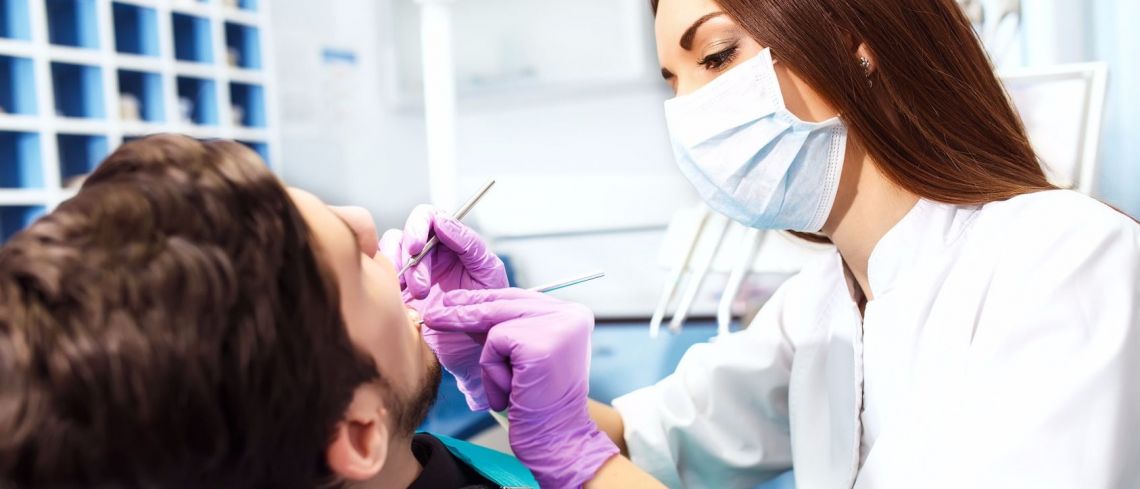
Our mouths speak volumes about our overall wellbeing, which is why the dental team is perfectly placed to improve your journey towards improving your overall health.
With the ‘drill and fill’ era of dentistry consigned to the history books, dental teams pay more than just lip service to the ideal of integrated health care.
These days, dentistry is less to do with invasive intervention and more to do with prevention – as well as any elective cosmetic treatments that may follow once the foundations are strong and healthy!
Teeth whitening, veneers, adult orthodontics and complete smile makeovers only ever work best when we have a healthy mouth, teeth and gums.
But, dental therapy and oral health education make natural bedfellows for nutritional advice, smoking cessation guidance and health promotion and there is a lot you can learn in a trip to the dental clinic.
Did you know we can now seek treatment from a dental hygienist or therapist without first having to see the dentist – widening our options massively when it comes to booking an appointment?
No longer confined to hospital and community settings, a dental therapist’s skills, in particular, demonstrate a holistic approach to care; their training based, as it is, on disease prevention.
Besides having an overarching responsibility for oral health care, there is also a legal and regulatory expectation for your dental professional to meet your overall health needs, with the profession’s regulatory body, the General Dental Council, maintaining that all aspects of our health and wellbeing should be considered at all times.
So, what does this mean for us? If the mouth is the window on our health – and there is a wealth of evidence to support this – then the health of our teeth and gums and their link to systemic diseases is an important issue.
Dental therapist and comparethetreatment oral health expert, Melonie Prebble, explains: ‘Regular dental examinations give us both the time and opportunity to detect early predictors of systemic disease as well as dental disease. Patients usually present at the practice when seemingly healthy, so we are on the frontline to find any “hidden’ problems” – an examination reveals a lot more than just the health of the oral cavity. Additionally, recording your medical history at every visit can highlight any risks and we can review habits jointly.’
Only last week a new study suggested our oral health was greatly influenced by factors other than diet – our gender, where we live, and our behaviour, for instance.
The research findings on the oral health of an African tribe who are shifting from a foraging, wild-food diet to an agriculture-based diet indicated that dental health is influenced by many factors.
Today is World Oral Health Day and it serves as a reminder of the importance of good oral hygiene habits, avoiding risk factors and having a regular dental check-up.
So, exactly what can the dental team learn from looking inside your mouth?
• Tooth erosion Acidic foods and drinks are well known sources of the problem; conditions such bulimia or anorexia nervosa can be, too.
• Cancer Excessive alcohol consumption and smoking both impact on oral health, besides the wider implications. The most significant contributory factors to oral cancer are smoking and heavy drinking, while the use of smokeless tobacco, chewing betal quid, and a poor diet can also increase the risk. Researchers have also found that men with gum disease were 49% more likely to develop kidney cancer, 54% more likely to develop pancreatic cancer, and 30% more likely to develop blood cancers.
• Diabetes Many cases of diabetes in the UK are undiagnosed and dentists have a useful role to play. Diabetic patients arrive in the dentist’s chair with their own set of clinical challenges and dental teams can help manage diets to control any negative impact it has on periodontal status. Some dental practices even offer screening opportunities in the form of blood glucose testing (BGT).
• Stress Stress can lead to serious damage to our teeth – an increase in erosive alcohol and a desire for more sugary food and drinks, for example. Stress may also cause bruxism (tooth grinding), which not only wears down teeth, but also increases the risk of developing other symptoms such as headaches, TMJ disorders, facial pain, ear pain and is associated with sleep apnoea.
• Childbirth Women with periodontal disease are believed to be more likely to deliver babies prematurely or with low-birth weight than mothers with healthy gums.
• Hypertension Oral hygiene may be considered an independent risk factor for hypertension and that maintaining good periodontal health habits may prevent and control the condition.
• Osteoporosis Because bone density decreases, we may lose the supporting bone of our teeth, which become loose or may fall out.
• Respiratory disease Bacteria in the oral cavity can be aspirated into the lungs and lead to pneumonia.
Get Oral Health Advice from Melonie Prebble
Related Treatments
Ceramic Fixed Braces
Ceramic braces are braces that are fixed to the te...

Damon Braces
Compared to normal orthodontics, Damon Braces use ...

Fastbraces
Fast Braces are a relatively new and innovative or...
Fixed Braces
Fixed braces are the most common type of orthodont...
Incognito Braces
While traditional braces, commonly referred to as ...

Inman Aligner
The Inman Aligner is a solution that helps to alig...

Invisalign
The Invisalign System straightens teeth using a se...
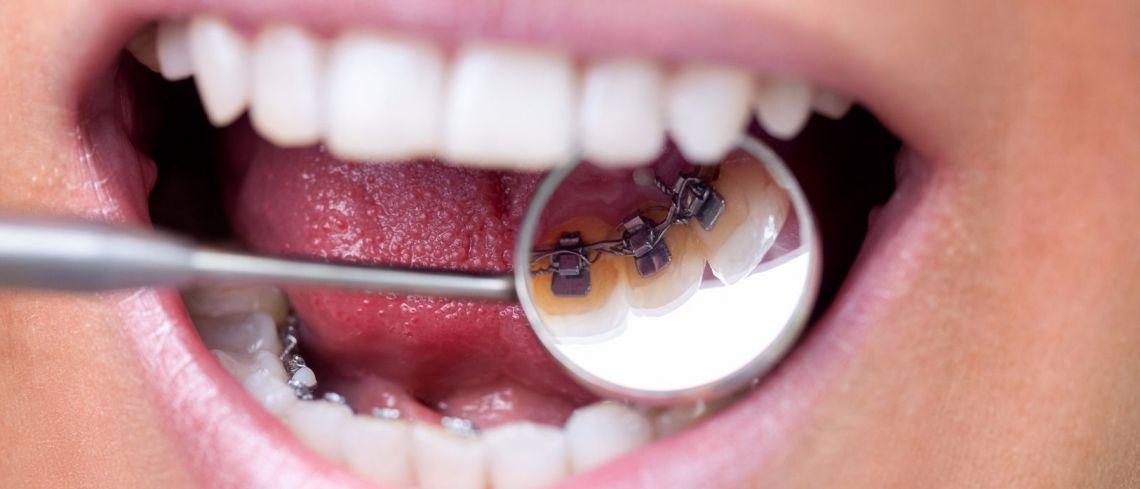
Lingual Braces
These devices are almost the same as fixed wire br...

Metal Fixed Braces
Metal brackets are linked together using wire and ...

Opalescence
The desire for pearly white teeth has caused tooth...
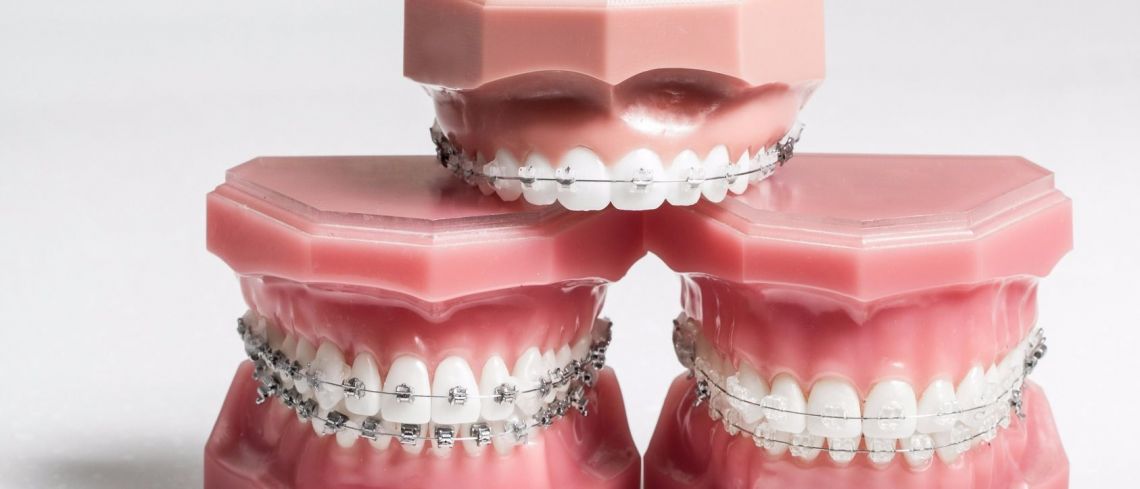
Orthodontics
Devices such as removable braces as clear aligners...

Philips Zoom
Philips Zoom teeth whitening is a unique procedure...
Quick Straight Teeth
If you are looking for straighter teeth, and ...
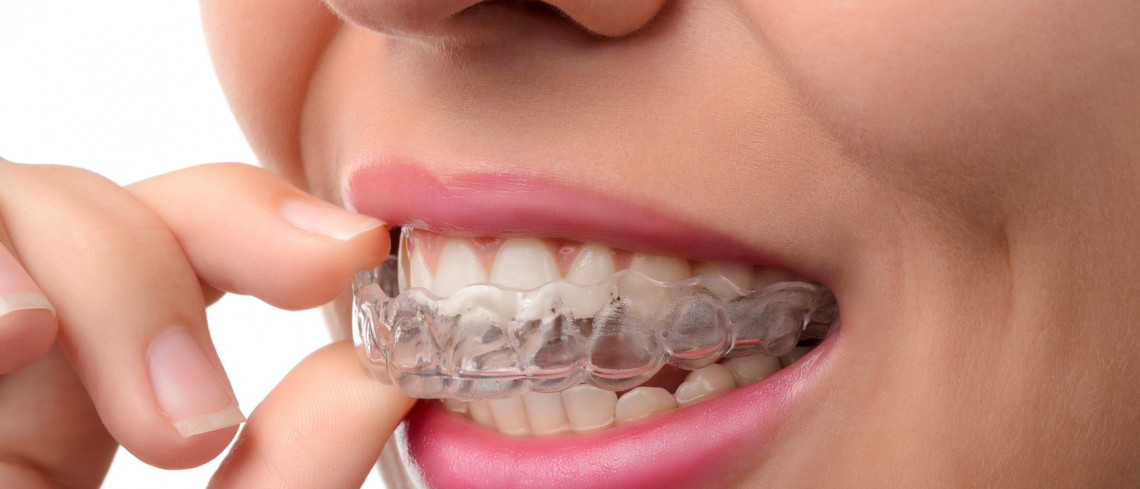
Removable Braces (Clear Aligners)
If your teeth require only small corrections to ma...

RXaligners
RXaligners are clear trays that can be removed. Th...

Six-Month Smiles
The Six-Month Smiles system can provide fast and e...

Smile Make Over
A Smile Makeover involves one or more cosmetic, de...
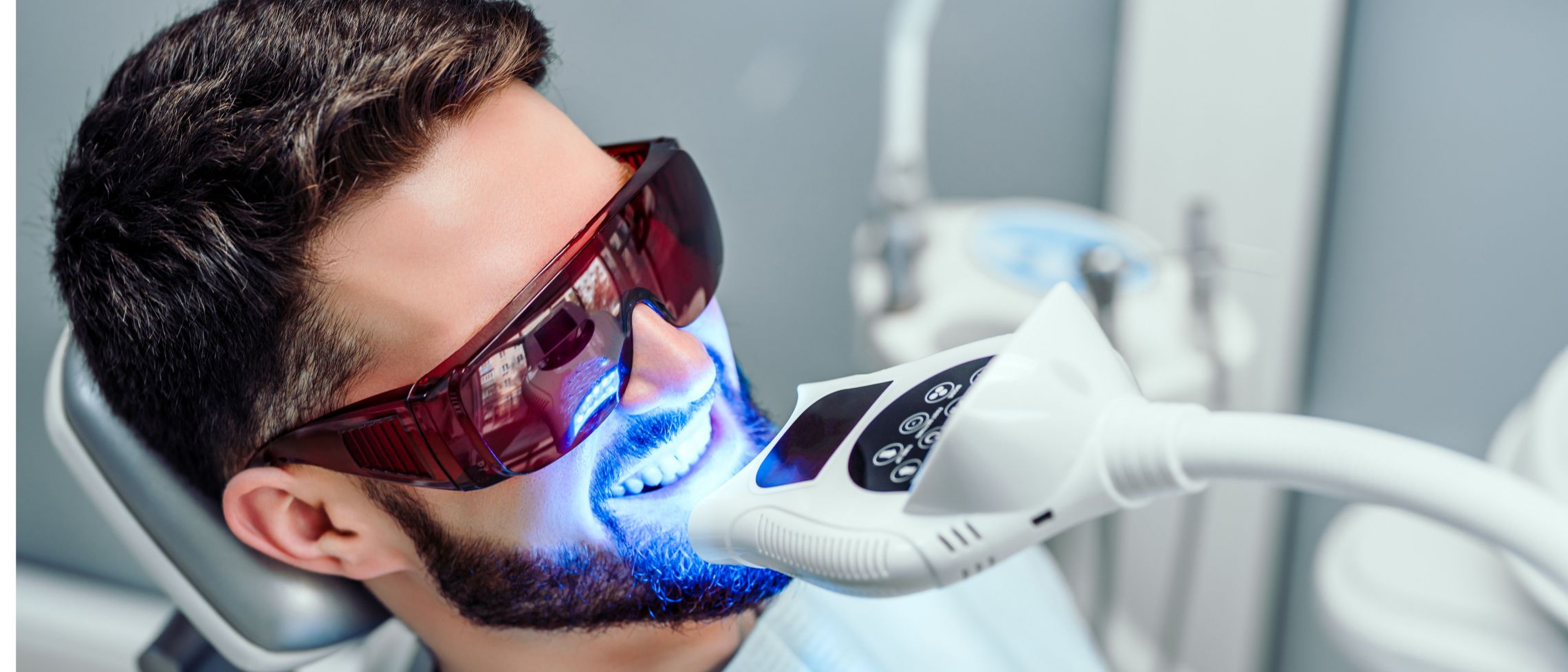
Teeth Whitening
Tooth whitening involves lightening the natural co...
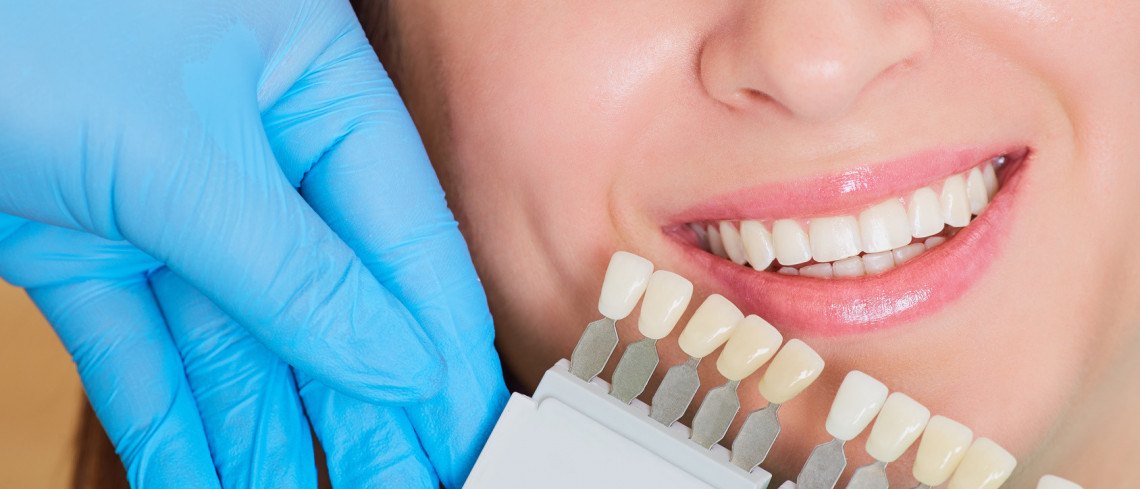
White Dental Beauty
So you have tried whitening toothpastes, over the ...